You push through the pain during a morning run. You assume it’s just a sore muscle. But weeks later, the ache is still there and getting worse. That nagging discomfort could be a hairline fracture, a small but serious crack in bone that millions of people unknowingly walk around with every day.
This guide gives you everything you need to know about a hairline fracture , without the medical jargon. Whether you’re a runner, an athlete, or someone who just had an awkward landing, read on.
1. What Is a Hairline Fracture?
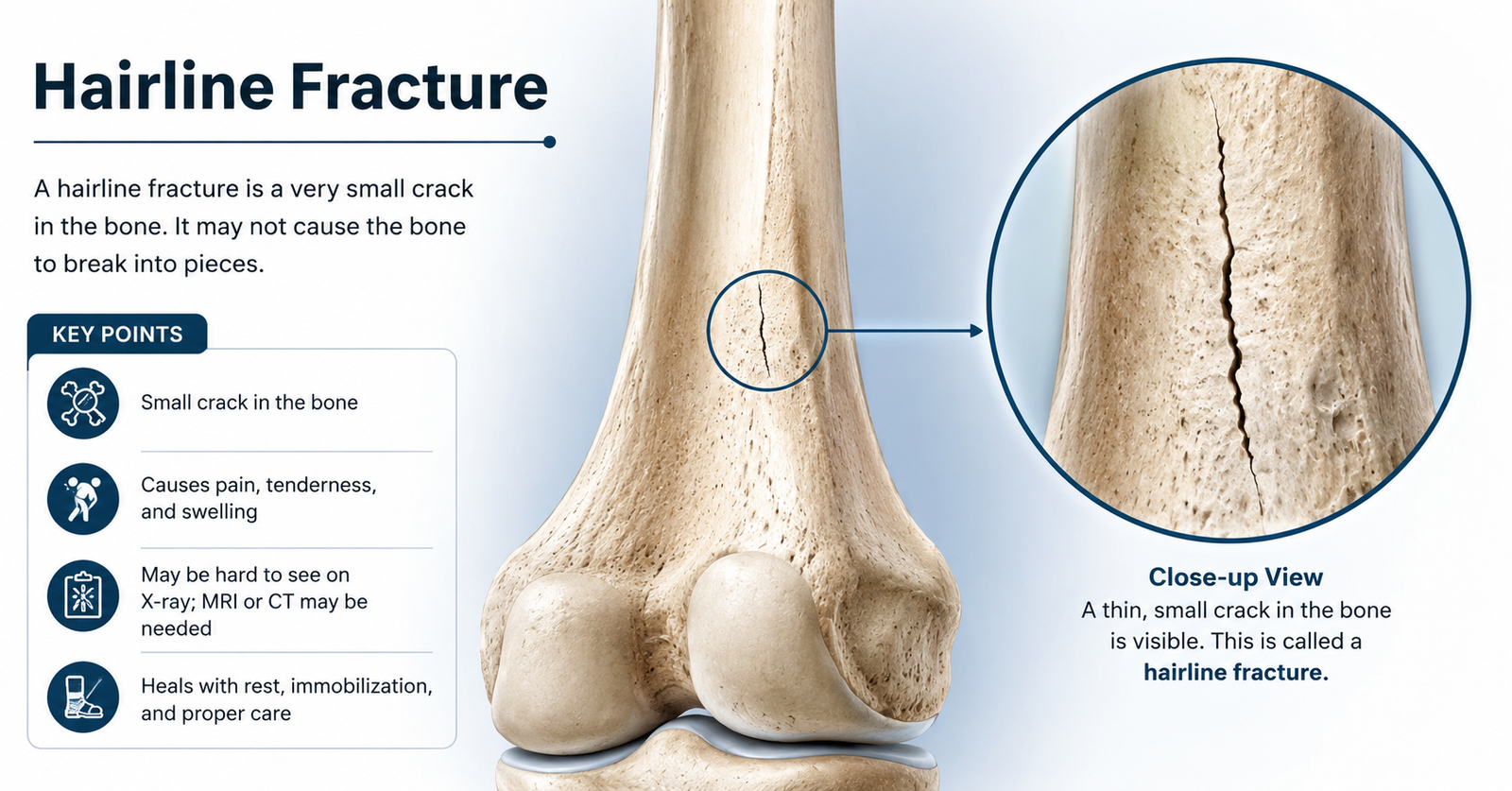
A hairline fracture is a thin, partial crack in a bone that doesn’t go all the way through. Unlike a complete fracture , where the bone snaps in two , a hairline fracture is subtle, often invisible to the naked eye, and easy to dismiss as a sprain or strain.
The term hairline comes from how the crack looks on imaging: as thin as a strand of hair. Medical professionals also call it a stress fracture, particularly when it results from repetitive pressure rather than a single trauma.
Hairline fractures are common in weight-bearing bones , the feet, ankles, shins, and hips , but they can occur anywhere in the body given enough force or repeated stress.
| ⚡ Key FactHairline fractures account for approximately 10–16% of all sports-related bone injuries. Runners and military recruits are among the highest-risk groups. |
2. Common Causes of a Hairline Fracture
There are two main ways a hairline fracture develops:
A. Repetitive Stress (Overuse Injuries)
This is the most common cause. When muscles become fatigued, they can no longer absorb shock effectively. The force then transfers to the bone, creating microscopic cracks over time. Classic examples include:
• Long-distance running without adequate rest
• Military training with sudden increase in physical load
• Gymnastics, basketball, and court sports
• Ballet dancing (especially on the metatarsals)
B. Sudden Impact or Trauma
A one-time event can also cause a hairline fracture , especially in someone with weakened bones:
• Awkward landing from a jump
• A hard tackle in contact sports
• Tripping and bracing a fall with the hand or wrist
| Risk Factor | Why It Increases Risk |
| Low bone density (osteoporosis) | Bones crack under less pressure |
| Sudden increase in activity | Bones not conditioned to handle new load |
| Poor nutrition (Vitamin D, Calcium deficiency) | Weaker bone structure overall |
| Improper footwear | Less shock absorption during impact |
| Previous stress fractures | Bone may not have fully healed or rebuilt |
| Female athletes (Female Athlete Triad) | Hormonal factors affect bone density |
3. Symptoms: How to Tell If You Have a Hairline Fracture
The tricky part about a hairline fracture is that the symptoms can mimic a sprain or soft tissue injury. Here’s what to watch for:
| Symptom | Description | Severity |
| Localized pain | Aches at a precise spot, not a general area | Moderate |
| Pain that worsens with activity | Improves with rest; returns when loading the area | Moderate–High |
| Tenderness to touch | Pressing on the bone hurts immediately | High (diagnostic) |
| Mild swelling | Area looks slightly puffed up or inflamed | Low–Moderate |
| Bruising (occasional) | May not appear at all, or show up days later | Variable |
| Pain that lingers | Doesn’t resolve like a muscle soreness would | High (red flag) |
Red Flag: If pain occurs even at rest or worsens significantly overnight, seek immediate medical attention. A hairline fracture left untreated can become a complete fracture.
4. Which Bones Are Most Commonly Affected?
While a hairline fracture can technically occur in any bone, certain locations are far more common , particularly in athletes and active individuals.
| Bone / Location | Most Common In | % of Stress Fractures |
| Tibia (shin) | Runners, military personnel | ~49% |
| Metatarsals (foot bones) | Dancers, runners, hikers | ~25% |
| Fibula (lower leg) | Distance runners | ~12% |
| Navicular (foot) | Sprinters, jumpers | ~6% |
| Hip / Femoral neck | Older adults, female athletes | ~5% |
| Spine (vertebrae) | Gymnasts, weightlifters | ~3% |
5. Diagnosis: What Doctors Actually Look For
Getting an accurate diagnosis is critical. Because a hairline fracture is so small, standard X-rays often miss them in the early stages.
Physical Examination
A doctor will press along the bone to find a precise ‘point of maximum tenderness.’ This fingertip pressure test is highly telling , a sprain typically hurts across a wider area, while a hairline fracture produces sharp pain at one precise spot.
Imaging Tests
| Test | Accuracy for Hairline Fracture | Notes |
| X-ray | Low (early stage) | May appear normal for 2–3 weeks; bone callus forms later |
| MRI | Very High | Best choice shows bone marrow edema and early cracks |
| CT Scan | High | Good for complex areas like the spine or hip |
| Bone Scan | High (non-specific) | Detects increased bone activity; less precise location |
MRI is considered the gold standard for diagnosing a hairline fracture, especially in the first 1–2 weeks when X-rays are often negative.
6. Treatment Options for a Hairline Fracture
The good news: most hairline fractures heal without surgery. The key is catching them early and following the right recovery protocol.
R.I.C.E. The First-Line Response
• Rest: Stop the activity causing pain immediately
• Ice: Apply for 15–20 minutes every 2–3 hours in the first 48 hours
• Compression: Gentle wrap to reduce swelling
• Elevation: Keep the affected limb raised above heart level when possible
Medical Treatment
| Treatment | When Used | Goal |
| Protective footwear / boot | Foot and ankle fractures | Offload pressure from the bone |
| Crutches | Lower limb fractures | Eliminate weight-bearing during healing |
| Cast or splint | Wrist, arm fractures | Immobilize to allow healing |
| Bone stimulator | Slow-healing fractures | Use low-level electrical pulses to speed bone repair |
| Surgery (rare) | High-risk locations (hip, navicular) | Internal fixation to prevent complete break |
| Calcium & Vitamin D supplements | Throughout recovery | Support bone repair and density |
Pain medication (NSAIDs like ibuprofen) should be used cautiously , some research suggests they may impair the bone healing process. Always consult your doctor before taking any medication for a hairline fracture.
7. Recovery Timeline: What to Realistically Expect
Recovery from a hairline fracture depends on location, severity, age, and your overall bone health. Here’s a general guide:
| Week | Stage | What’s Happening |
| 1–2 | Acute Inflammation | Pain, swelling; bone begins forming early repair cells |
| 3–4 | Early Bone Repair | New bone tissue (callus) starts bridging the crack |
| 5–6 | Bone Bridging | Callus hardens; pain decreases significantly |
| 7–8 | Remodeling Begins | Bone remodels to original shape; return to light activity |
| 8–12 | Full Recovery | Most patients return to full activity with doctor clearance |
| 12+ | High-Risk Fractures | Hip and navicular fractures may take longer (3–6 months) |
Important: Returning to activity too early is the single biggest cause of re-injury or complete fracture. Always get imaging confirmation before resuming sports.
8. How to Prevent a Hairline Fracture
Prevention is far better than a 6-week boot. Here’s how to protect your bones proactively:
Training Smart
Follow the 10% rule: never increase weekly mileage or intensity by more than 10% at a time
Incorporate rest days , bone needs time to remodel between hard sessions
Cross-train to reduce repetitive loading on the same bones
Nutrition & Bone Health
• Consume 1,000–1,200 mg of calcium daily (dairy, leafy greens, fortified foods)
• Maintain Vitamin D levels (sun exposure + supplementation if deficient)
• Avoid crash diets , calorie restriction reduces bone density, especially in female athletes
Gear & Biomechanics
• Replace running shoes every 300–500 miles
• Consider custom orthotics if you have flat feet or high arches
• Get a running gait analysis if you’re a high-volume runner
9. Hairline Fracture vs. Stress Fracture vs. Complete Fracture
These terms often cause confusion. Here’s the clearest comparison:
| Type | Cause | Bone Involvement | Healing Time | Surgery? |
| Hairline / Stress Fracture | Repetitive overuse | Partial crack, bone intact | 6–12 weeks | Rarely |
| Complete Fracture | Acute trauma (fall, impact) | Bone fully broken | 6–26 weeks | Often |
| Avulsion Fracture | Sudden muscle pull | Small fragment pulled off | 4–8 weeks | Sometimes |
| Compression Fracture | Axial load (spine) | Bone collapses on itself | 8–16 weeks | Rare |
The Bottom Line
A hairline fracture is your body’s way of saying it has been pushed past its limits. Respect that signal. The difference between a 6 week recovery and a 6-month nightmare is simply whether you act early.
If you have persistent, localized bone pain that worsens with activity and doesn’t resolve with typical rest , don’t assume it’s a muscle issue. Get it checked. An MRI takes an hour; ignoring a hairline fracture can cost you a season.